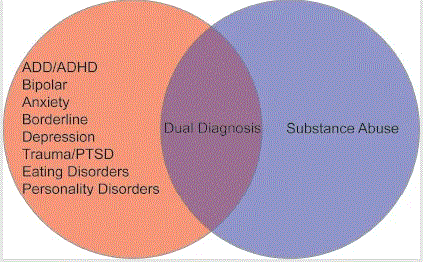
What Is Dual Diagnosis? And It’s Link to Addiction Disorders?
A person with a dual diagnosis has both an alcohol or drug problem and a mental health disorder. These conditions happen together frequently. About half of people who have a mental illness will also have a substance use disorder at some point in their lives and vice versa. The interactions of the two conditions can worsen both.
According to the National Center for Biotechnology Information (NCBI) [1], the dual diagnosis was first identified in the 1980s among individuals with coexisting severe mental illness and substance abuse disorders. Today, the Substance Abuse and Mental Health Services Administration (SAMSHA) uses the term co-occurring disorders (COD) to refer to the aforementioned concurrent disorders.
Why Do Substance Use Disorders And Mental Disorders Occur Together? An Explanation Of Dual Diagnosis
Even while both issues frequently coexist, even if one showed up first, this does not imply that it caused the other. In actuality, determining which came first might be challenging. According to researchers, there are three possible explanations for why they co-occur:
- Both substance use disorders and mental problems may be influenced by common risk factors. These elements include trauma, stress, and genetics.
- Drug usage and substance use disorders can be influenced by mental problems. For instance, individuals with mental illnesses may take medications or alcohol in an effort to momentarily feel better. Self-medication is referred to as this. Additionally, mental illnesses may alter your brain in a way that increases your risk of developing an addiction.
- Addiction to drugs and alcohol as well as substance use can cause mental disorders to emerge. The use of drugs or alcohol may alter the brain in ways that increase your risk of developing a mental illness.
What Are The Treatments For Dual Diagnosis?
A person with two diagnoses must manage both ailments. You must give up alcohol and drugs for the treatment to be effective. Medicines and behavioral therapy are possible treatment options. Assistance groups can also provide you with social and emotional support. They serve as a forum for exchanging advice on how to handle everyday difficulties.
Skip to:
- What Is Dual Diagnosis? And It’s Link to Addiction Disorders?
- Why Do Substance Use Disorders And Mental Disorders Occur Together? An Explanation Of Dual Diagnosis
- What Are The Treatments For Dual Diagnosis?
- What Are The Causes Of Dual Diagnosis?
- What Is The Dual Diagnosis Definition?
- Signs Of A Dual Diagnosis Or Co-Occurring Disorder
- Statistics On Dual Diagnosis
- Why Is Self-Medication Dangerous?
- Dual Diagnosis Treatment Center
- Dual Diagnosis Treatment Centers NJ
Learn more:
- Inpatient Alcohol Rehab
- Inpatient Drug Rehab
- Substance Abuse Treatment Center
- Benefits of Treating Drug Addiction
- Substance Abuse Defined, Signs, Symptoms, Link to Mental Health
- Connection Between Alcohol And Depression, Causes, Statistics, Signs and Symptoms
- PTSD And Addiction Strong Connection
- Alcohol And Anxiety Co-Occurring Mental Health Disorder
- Mental Health Services
- Anxiety Medication and Alcohol
What Is The Dual Diagnosis Definition?
Dual diagnosis or co-occurring disorders (COD) is defined as co-occurring substance-related and mental disorders. People said to have co-occurring disorders have one or more substance-related disorders as well as one or more mental disorders.
According to the National Institute on Alcohol Abuse and Alcoholism (NIAAA) [3], in the current Diagnostic and Statistical Manual of Mental Disorders (DSM), alcohol use disorder (AUD) and other substance use disorders are defined as psychiatric disorders. Many people who misuse alcohol also abuse other drugs, and vice-versa. Additionally, other psychiatric disorders often co-occur with substance use disorder. This is referred to as co-morbidity. Dual diagnosis, co-occurring disorders, and co-morbidity are interchangeably used today.

People with a dual diagnosis require an integrated treatment plan that addresses both disorders as interconnected issues. According to the National Survey on Drug Use and Health (NSDUH), 45% of people with substance use disorders have a co-occurring mental health disorder. By seeking treatment for addiction and co-occurring behavioral and mental health disorders, you can work on successfully attaining the fulfilling and healthy life you deserve.

Get Your Life Back
Find Hope & Recovery. Get Safe Comfortable Detox, Addiction Rehab & Mental Health Dual Diagnosis High-Quality Care at the We Level Up Treatment Centers Network.
Hotline (877) 378-4154Top 10 Dual Diagnosis FAQs
-
What Is Dual Diagnosis Rehab?
If you are wondering, “what is dual diagnosis treatment?”, the answer is that dual diagnosis meaning is when a person has both a mental illness and a substance use disorder at the same time, it’s referred to as having a dual diagnosis (also known as a co-occurring disorder) and typically gets dual diagnosis therapy to get the treatment they need for a safe recovery journey.
-
What Are Common Types Of Dual Diagnosis Treatments?
Treatment for dual diagnosis. A person with two diagnoses must manage both ailments. You must give up alcohol and drugs for the treatment to be effective. Medicines and behavioral therapy are possible treatment options. Assistance groups can also provide you with social and emotional support.
-
What Are Dual Diagnosis Inpatient Treatment Centers?
According to research, individuals with a dual diagnosis benefit from integrated treatment plans in inpatient dual diagnosis treatment centers that address both their mental illness and substance abuse. Treatment can assist individuals in residential dual diagnosis treatment centers in controlling their alcohol or drug use, enhancing their physical and emotional well-being, and enhancing their overall functioning in dual diagnosis centers. Dual diagnosis residential treatment is a great way to get the care that you deserve for your recovery journey.
-
What Is Dual Diagnosis AA/DRA?
DRA (Dual Recovery Anonymous/Dual Diagnosis Anonymous) was created to support both men and women who have dual conditions. When a person has both a psychiatric or emotional disorder and a drug dependency, this is known as a dual disorder. relapse, as well as to spread the word of recovery to other people who suffer from a dual disease during their dual diagnosis AA meetings.
-
What Are The Signs That Someone Needs To Be In A Dual Diagnosis Program?
A person with a dual diagnosis has both a co-occurring substance use disorder and a mental illness. Clients can discover more about the symptoms of a dual diagnosis condition through the best dual diagnosis treatment center North Carolina rehabs have to offer. When people start withdrawing from their ties to their family and friends, that is one of the first signs of a problem. The person could also struggle to control their usage of drugs or their everyday chores.
-
What Happens In A Typical Dual Diagnosis Group Therapy Session?
Substance use disorders, mental health issues, and trauma healing are all treated with group therapy. Due to this, group therapy is frequently used in dual-diagnosis addiction treatment facilities. Although group therapy has numerous advantages, its effectiveness greatly depends on each patient’s willingness to engage.
-
What Is The Difference Between Dual Diagnosis Vs Co-Occurring Disorders?
If you are wondering, “what is the difference between dual diagnosis vs co occurring disorders?”, the answer is the phrase “dual diagnosis treatment” is now most frequently used to refer to the approach taken to treat people who suffer from both mental illness and addiction. The term “co-occurring disorders” refers to a number of illnesses that frequently coexist with drug or alcohol addiction.
-
What Are Holistic Dual Diagnosis Treatment Centers?
If you are wondering, “what is a dual diagnosis treatment center for holistic methods?”, the answer is in order to develop a thorough treatment plan for substance use disorders, rehab centers that use holistic methodologies typically carefully evaluate an integrated physical, mental, and spiritual model. Some of these methods, some of which are based on culturally traditional practices, are also labeled as alternative or supplementary treatments.
-
What Is The Typical Dual Diagnosis Recovery Process?
A person with two diagnoses must manage both ailments. You must give up alcohol and drugs for the treatment to be effective. Medicines and behavioral therapy are possible treatment options. Assistance groups can also provide you with social and emotional support.
-
How Long Is Long Term Dual Diagnosis Treatment Centers?
90 days
What Are The Causes Of Dual Diagnosis?
Although an alcohol or drug problem and a mental disorder often happen together, this does not mean that one caused the other, even if one appeared first. In fact, it can be challenging to distinguish which came first. According to the National Institute of Health (NIH) [2], researchers think that there are three possibilities as to why they happen together:
- Common risk factors may contribute to both mental disorders and substance use disorders. These factors include genetics, stress, and trauma.
- Mental disorders can contribute to drug use and substance use disorders. For example, people with mental disorders may use drugs or alcohol to try to feel better temporarily. This is known as self-medication. Also, mental disorders may change the brain to make it more likely you will become addicted.
- Substance use and addiction can contribute to the development of a mental disorder. Substance use may change the brain to make you more likely to develop a mental illness.
What Causes Substance Use Disorder?
Like many mental health disorders, several factors may contribute to the development of alcohol or drug addiction. The main factors are:
Environment
- Environmental factors, including your family’s beliefs and attitudes and exposure to a peer group that encourages drug use, seem to play a role in initial drug use.
Genetics
- Once you’ve started using a drug, the development into addiction may be influenced by inherited (genetic) traits, which may delay or speed up the disease progression.
Get Help. Get Better. Get Your Life Back.
Searching for Accredited Drug & Alcohol Rehab Centers Near You? Or Mental Health Support?
Even if you have failed previously, relapsed, or are in a difficult crisis, we stand ready to support you. Our trusted behavioral health specialists will not give up on you. Call us when you feel ready or want someone to speak to about therapy alternatives to change your life. Even if we cannot assist you, we will lead you wherever you can get support. There is no obligation. Call our hotline today.
FREE Addiction Hotline – Call 24/7What Causes Mental Illness?
Most mental conditions don’t have a single cause. Instead, they have a variety of causes, called risk factors. The more risk factors someone has, the more likely they are to develop a mental illness. Sometimes, mental illness develops gradually. Other times, it doesn’t appear until a stressful event triggers it.
There are many risk factors and triggers, but here are a few examples:

Genetics
- Mental illness often runs in the family.
Environment
- Living in a stressful environment can make you more likely to develop a mental illness. Things like living in poverty or having an abusive family put a lot of stress on your brain and often trigger mental illness.
Mental Health Dual Diagnosis FAQs
What are common dual diagnosis examples?
A dual diagnosis mental health diagnosis occurs when a person has both a mental disorder and a drug addiction. For instance, you can be dealing with both alcoholism and melancholy at the same time. These problems could get worse if left untreated.
What Is The Connection Between Bipolar And Borderline Personality Disorder Dual Diagnosis?
There is an estimated 20% overlap in diagnostic frequency, according to several reviews. In other words, roughly 20% of people with bipolar disorder also have BPD, and similarly, 20% of those with BPD also have bipolar disorder. Therefore, even though they make up a small percentage of patients, those who have comorbid diagnoses are significant.
What Is The Best Treatment That A Dual Diagnosis Psychiatrist Can Provide?
Integrated intervention, in which a person receives dual diagnosis services and therapy for both their documented mental illness and substance dependence, is the best form of treatment for dual diagnoses. It is no longer valid to say, “I cannot treat your depression because you also drink,” because both problems need to be addressed, according to modern thinking.
Childhood trauma
- Even if you’re no longer in a stressful environment, things that happened to you as a child can have an impact later in life.
Stressful events
- Like losing a loved one, or being in a car accident.
Negative thoughts
- Constantly putting yourself down or expecting the worst can get you stuck in a cycle of depression or anxiety.
Unhealthy habits
- Like not getting enough sleep, or not eating.
Drugs and alcohol
- Abusing drugs and alcohol can trigger a mental illness. It can also make it harder to recover from mental illness.
Brain chemistry
- Mental illness involves an imbalance of natural chemicals in your brain and your body.
These risk factors don’t just affect who will develop a mental illness in the first place. They also affect how severe their symptoms will be, and when they will experience those symptoms.
Signs Of A Dual Diagnosis Or Co-Occurring Disorder
The signs of a dual diagnosis vary greatly between people. Typically, symptoms will depend on the type of drug or substance abuse as well as the severity of the co-occurring condition.
Symptoms of a dual diagnosis include:
- Sudden changes in general behavior
- Difficulty managing daily tasks and responsibilities
- Avoiding events or social activities that were once enjoyed
- Neglecting health and hygiene
- Delusional thinking or cognitive impairments
- Refusal to seek or comply with treatment
- Mentions of thoughts of suicide or suicidal behaviors
- Erratic and impulsive behaviors
- Issues managing finances
- Poor performance at school or work
Statistics On Dual Diagnosis
Who is affected?
- According to the National Institute on Drug Abuse [4], 7.7 million adults have co-occurring mental and substance use disorders. This doesn’t mean that one caused the other and it can be difficult to determine which came first.
- Of the 20.3 million adults with substance use disorders, 37.9% also had mental illnesses.
- Among the 42.1 million adults with mental illness, 18.2% also had substance use disorders.
First-class Facilities & Amenities
World-class High-Quality Addiction & Mental Health Rehabilitation Treatment
Rehab Centers TourRenowned Addiction Centers. Serene Private Facilities. Inpatient rehab programs vary.
Addiction Helpline (877) 378-4154Proven recovery success experience, backed by a Team w/ History of:
15+
Years of Unified Experience
100s
5-Star Reviews Across Our Centers
10K
Recovery Success Stories Across Our Network
- Low Patient to Therapist Ratio
- Onsite Medical Detox Center
- Comprehensive Dual-Diagnosis Treatment
- Complimentary Family & Alumni Programs
- Coaching, Recovery & Personal Development Events
Who gets treatment?
There are many effective treatments for both mental and substance use disorders. A comprehensive treatment approach will address both disorders at the same time.
Not everyone with co-occurring conditions gets the treatment they need:
- 52.5% of those with dual diagnosis conditions received neither mental health care nor substance use treatment.
- 34.5% of those with dual diagnosis conditions received mental health care only.
- 09.1% of those with dual diagnosis conditions received both mental health care and substance use treatment.
- 3.9% of those with dual diagnosis conditions received substance use treatment only.
Individuals who struggle with mental health disorders either seek clinical medication or self-medicate with drugs and alcohol. People that get prescriptions for their condition are less likely to develop abuse disorders, but often the medications that they get access to have high abuse potential, creating more risk.
People that self-medicate for their mental illnesses often start early, and the use of drugs or alcohol as a way to escape becomes a natural part of life.
The reverse order can also be true, in which a mental disorder is caused or worsened by the use of drugs or alcohol. For example, some common pairings. A study found that cocaine use can cause paranoia and anxiety:
Why Is Self-Medication Dangerous?
When a person has a problem with mental illness and substance use, they need to seek out the best dual diagnosis treatment program. Often, individuals use drugs and alcohol to self-medicate for their mental illness. These drugs only make them feel better temporarily. Because the effects wear off, the person has to use it repeatedly to relieve the symptoms of their mental conditions.
Self-medication is dangerous because it can lead to addiction or even an overdose. It also makes treatment harder because the person has to treat addiction and mental illness. If they do not treat both problems at a dual diagnosis treatment center, they are more likely to relapse.
According to the Substance Abuse and Mental Health Service Administration (SAMHSA) [5], no specific combinations of mental and substance use disorders are defined uniquely as co-occurring disorders. Some of the most common mental disorders include:
People being treated for mental disorders also often misuse the following types of substances:
- Alcohol
- Tobacco
- Opioids
- Stimulants
- Marijuana
- Hallucinogens
- Prescription drugs
World-class, Accredited, 5-Star Reviewed, Effective Addiction & Mental Health Programs. Complete Behavioral Health Inpatient Rehab, Detox plus Co-occuring Disorders Therapy.
CALL (877) 378-4154End the Addiction Pain. End the Emotional Rollercoaster. Get Your Life Back. Start Drug, Alcohol & Dual Diagnosis Mental Health Treatment Now. Get Free No-obligation Guidance by Substance Abuse Specialists Who Understand Addiction & Mental Health Recovery & Know How to Help.
Dual Diagnosis Treatment Center
Treating dual diagnosis clients is a critical aspect of our inpatient treatment experience because co-occurring disorders are strongly connected with instances of substance abuse. Creating a treatment plan that addresses the physical aspects of withdrawal, the psychological connection with drug use, and addressing underlying mental health disorders is all a part of setting clients up for success during the treatment of dual diagnosis.
A thorough mental health analysis identifies opportunities for treatment. Meeting with mental health counselors and medical care providers means access to behavioral therapy and medication treatment. Proper treatment leads to change for better, healthier living.
The treatment centers for dual diagnosis may use different therapies like cognitive behavioral therapy or trauma therapy to help the individual to change their lifestyle. Group meetings help provide feedback, advice, and support during recovery. Meanwhile, family therapy allows clients to get the support they need to stay sober after their rehab stay is complete.
Dual Diagnosis Treatment Centers NJ part of the We Level Up Nationwide Network
We Level Up NJ and our top-rated dual diagnosis treatment centers believe that if the client can identify the underlying issue and treat it simultaneously with their treatment for addiction, the client’s chances of a successful, relapse-free recovery are much improved. In fact, once we can identify and properly begin treatment on the underlying issue that’s driving or co-occurring with the dependency on alcohol or other drugs, clients will have reached a major milestone and will be that much closer to long-term sobriety.

We Level Up NJ do not believe that long-term recovery comes in a one-size-fits-all program. For this reason, each client, upon arrival at our drug treatment center, will undergo extensive and comprehensive dual diagnosis exams which include physical and psychological tests with our team of physicians, mental health specialists, spiritual advisers, and nutritionists.
Together, we will determine what the client’s underlying issues are so we can then customize an individualized approach and, when appropriate, provide integrated dual diagnosis treatment. The symptoms of the multiple disorders that can occur alongside addiction can present complex and similar symptoms. Proper diagnosis requires a highly trained professional staff with years of experience in dual diagnosis treatment programs.
Looking for dual diagnosis treatment centers New Jersey or Florida to California? Call one of our addiction specialists to learn more about our dual diagnosis treatment centers in Florida.
Seeking for dual diagnosis treatment centers California? Call one of our west coast addiction specialists to learn more about our dual diagnosis treatment facilities in California.
Learn more about the We Level Up dual diagnosis treatment centers network. Below are select popular destinations for our dual diagnosis programs.
We Level Up New Jersey

Licensed, Accredited w/ 100s of 5-star reviews.
- Addiction rehab center
- Detox center
- Dual diagnosis rehab center
We Level Up Lake Worth

Licensed, Accredited w/ 100+ 5-star reviews.
- Addiction rehab center
- Detox center
- Dual diagnosis rehab center
We Level Up Fort Lauderdale

Licensed, Accredited w/ 5-star reviews.
- Mental health center
- Depression, anxiety, trauma treatment
- Dual diagnosis rehab programs
Experience Transformative Recovery at the We Level Up Treatment Center.
See our authentic success stories. Get inspired. Get the help you deserve.



Start a New Life
Begin with a free call to an addiction & behavioral health treatment advisor. Learn more about our dual-diagnosis programs. The We Level Up treatment center network delivers various recovery programs at each treatment facility. Call to learn more.
- Personalized Care
- Caring Accountable Staff
- World-class Amenities
- Licensed & Accredited
- Renowned w/ 5-Star Reviews
We’ll Call You
Search We Level Up NJ Dual Diagnosis Resources
Sources:
[1] NCBI – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2880934/
[2] NIH – https://medlineplus.gov/dualdiagnosis.html
[3] NIAAA – https://www.niaaa.nih.gov/alcohols-effects-health/special-populations-co-occurring-disorders/other-psychiatric-disorders
[4] NIDA – https://www.drugabuse.gov/drug-topics/trends-statistics/infographics/comorbidity-substance-use-other-mental-disorders
[5] SAMHSA – https://www.samhsa.gov/medication-assisted-treatment/medications-counseling-related-conditions/co-occurring-disorders
[6] We Level Up – Dual Diagnosis Treatment
SAMHSA. (2015). Behavioral Health Trends In The United States: Results From The 2014 National Survey On Drug Use And Health. Retrieved on September 16, 2021, from: https://www.samhsa.gov/data/sites/default/files/NSDUH-FRR1-2014/NSDUH-FRR1-2014.pdf
National Institute On Drug Abuse. (2014). Severe Mental Illness Tied To Higher Rates Of Substance Use. Retrieved on September 16, 2021, from: https://www.drugabuse.gov/news-events/news-releases/2014/01/severe-mental-illness-tied-to-higher-rates-substance-use
National Institute On Drug Abuse. (2010). Comorbidity: Addiction And Other Mental Illnesses. Retrieved on September 16, 2021, from: https://www.drugabuse.gov/sites/default/files/rrcomorbidity.pdf
Innovations In Clinical Neuroscience. (2011). Substance Use Disorders And Borderline Personality. Retrieved on September 16, 2021, from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3196330/